Journey into the world of hyperemesis gravidarum
We're off on Holiday

After a very difficult start to the year Me and my HG Heroes are heading off into the Canadian Wilderness for 10 days to enjoy some much needed family time.
We wont have access to WiFi or phone signal, I will reply to any messages and emails during the first week of September.
If you are ordering items from my shop then please be aware they will NOT be dispatched until W/C 29th August.
If you need information and support please register for the Pregnancy Sickness Support Forum by clicking here where you will be in contact with trained Peer Supporters.
Dont forget you can book your tickets for ICHG2017 - the 2nd International Colloquium on Hyperemesis Gravidarum by visiting the website www.ichg2017.org
See you in September!
Fifty Shades of Green
Have a baby they said, you'll glow they said.
So I did but I didn't.
My glow was more a shade of pond green algae rather than the pregnant lady radiance I had hoped for.
It’s amazing how you know early on when everything's about to change and not just because your boobs are massive, it all proceeds with a puke.
Jamaica Baby! Literally on our ‘oneymoon’. We'd made it a year and so decided to jet off to Montego Bay in celebration. A trip to Bob Marley’s birthplace in Nile Miles and several undignified pee stops by the side of the road did make me wonder, the fuller chest, the spotting which I thought was a UTI (sorry for the TMI) and a pukey 10 hour flight home mistaking sickness for overindulgence and jet lag for what was about to become my hyperemesis hell.
Except I didn't have a bloody clue what hyperemesis was or that it even existed! Little did I know I’d go on to become a ‘professional puker”.
I was pregnant, I just knew it. The second line appeared as I sat on the loo laughing nervously. I needed digital confirmation, 2-3 weeks it told me!
Fuck a duck!
Must inform the husband, he was working away so I rang him up (never call him, he always calls me) I've always been high maintenance. He thought someone had died, and I did a little along the way.
Anyway he's delighted, we did say we'd try. I can tell he's gutted not to be trying more often, trying for longer, but he's chuffed everything’s in good working order! Every macho cloud and all that. By the time he's back home I must be about 6 or 7 weeks and we laugh at my first puke - ah that's the morning sickness kicking in we chuckle, all pregnant and smug together!
I look back at this memory and hate us both!
Then the fog descends, the nausea, the vomiting and not just in the morning but all the live long day! It's like the worst hangover known to woman (and I've had some belters) or think of food poisoning which lingers for 9 whole months!
I naively thought 'this is how it must be' until I couldn't get off the bathroom floor, until my piss was the colour of petrol, until I couldn't even sip water. Husband knew this was wrong, this was not normal morning sickness.
I lay across the blue plastic chairs of the A&E department with zero fucks to give. I looked like a homeless wreck, a drunk, a junkie even but I'd lost the will to care. Anything would’ve been better than this! They tested my urine - ketone levels were high, I was seriously dehydrated. They were lucky I managed to produce any urine in the first place - it really was taking the piss, they got a dribble at best.
Next I was scanned for multiples, we were equally terrified and excited somehow at the prospect of this! It would have saved me the head fuck of considering another potential HG pregnancy to have BOGOF babies first time round.
Alas there was no multiples as the 7 week scan showed what I declared was a single prawn in my womb. I called it a ‘wee bugger’, the midwife called it a parasite (she was on my side). It was healthy, heart beat visible on the screen and it was sucking the life out of me. There was love and relief but I still felt like I was dying. I can relate to Bella in Breaking Dawn (if there's any twihards reading this you'll get my meaning).
So I'm hooked up to IV fluids, I have a memory of sharing a IV stand with some other poor soul who just stepped out a lift. We looked like the walking dead, the stand was the only thing holding us up.
They gave me the cheap anti emetics first and they only made me sicker (the irony)! Zofran literally saved me, Zofran (or ondansetron), an expensive anti emetic usually reserved for chemo patients is pretty much the last resort. Those tiny yellow pills were priceless and now I had new sympathy for addicts.
Zofran helped reduce the puke sessions but the nausea never, ever let up, or the excessive spit (could fill a bucket) or the extreme sensitivity to smell. I couldn't even stand the smell of my own skin, I sprayed perfume on myself before bed and I'd became allergic to husband. Poor guy!
I had my prawn pic to keep me company in hospital on my first admission and I looked at it closely trying to figure out what the hell it was.
A fetus, a parasite, my vampire baby, my little love.
This was the standard chat that followed. ‘Get to twelve weeks and you’ll be fine’, what lies! ‘Ok it’s got to be better at sixteen weeks’, nope! There is no sense of time when you’re in the HG zone, it’s timeless, minutes, hours, days mean nothing. I didn’t even bother to hope for better, I knew it wouldn’t come. I firmly believe HG is the biggest endurance test known to woman. I sat zombie like for the duration. I went off the grid with some not knowing I was pregnant until after the baby arrived. Daytime TV proved to be a mild distraction. Murder She Wrote (which I’d never given the time of day) was a firm favourite. I could figure out a crime scene in less time than Jessica Fletcher, I was embarrassed for us both. It was my fate that I would endure HG for the whole nine months, little love did make an appearance five days early which was a welcome relief of sorts.
Now as much as I was grateful for the Zofran and the doctor who prescribed it, his name was actually Dr Love and I did love him, it left me feeling rather bagged up. Constipation is the curse of the Zofran. They’d given me the usual stool softeners to combat this but of course an HG sufferer is going to puke that stuff straight back up. So, no, the constipation along with the sickness and nausea was my constant companion. By Christmas I was six months pregnant and I’m not sure if the bump was all baby or due to a blockage. The best Christmas gift that year would’ve been the ability to have a crap. I’d googled (as you do) how to alleviate this horrendous situation. Take a warm bath said one website, I knew what this meant – and I did not fancy a festive floater. Lay on your side on the floor with a towel advised another site and so that is what I did. Christmas Day and there I lay on the bathroom tiles, on my side with a towel underneath my arse, husband was thankfully completely oblivious in another room. How undignified I thought as I pulled my knees up to my chest and hoped for the best. The bathroom floor was the scene of many a crime, if I wasn’t hugging the toilet I was laying on the floor as it’s alternative but it worked!
It was a very Merry Christmas!
Prawn baby was now affectionately named Hubble, being the nosey bastards we are husband and I paid for a gender scan. I’d always had a thing for Hubble Gardner (Robert Redford in The Way We Were) and Hubble rhymed with trouble which prawn baby had been nothing but. You can’t resent your unborn child (actually you can, so don’t feel bad about that) but you can resent the situation you find yourself in. I didn’t know Hyperemesis Gravidarum existed until it was written on my notes, until a kindly doctor knew I wasn’t functioning the way a normal pregnant woman should. Before Dr Love, I’d been to see a few GP’s during emergency appointments, sadly I don’t think many of them knew much about it either. One floaty female GP in tie dye told me to persevere as it wouldn’t last much longer. Where was the solidarity? I got back to the car and punched the dashboard in frustration at the ‘fucking hippie’ much to husband’s amusement.
The next GP told me to go straight to A&E and that’s how I knew I was ill and not just pregnant.
The last few months passed by in much the same way, still vomiting and still nauseated. The nausea was worse than the puking. Husband said he could tell what stage I was at in the puke zone by the tone of my vomit groans. The nausea was all consuming, I gained great skill at staring into space, sometimes I didn’t want to talk, sometimes I wanted to maintain the art of silence forever. It’s a lonely place to be, even when you’re harboring a tiny human life inside of you, when you’re puking for two instead of eating for two. Hyperemesis is a solitary affair.
March was the month of deliverance. I’d managed to practice the art of hypno birthing and found the meditations quite soothing so I was ready. I had my birth plan in place and consultant led care so I knew all would be well. I also knew the sickness and nausea had to go when baby arrived. I was so ready for this!
The labour was actually quite liberating. It was a Saturday and I’d had what husband and I later referred to as ‘the last supper’ - some Italian food that I managed to keep down. It was absolutely delicious and miraculous, it was obviously the fuel I would need for getting through the next twenty four hours. Propped in my usual space on the sofa which now had indentations the shape of my arse, I settled down to watch Ant & Dec’s Saturday Night Takeaway (doesn’t everyone)? They’d proudly re-released “Let’s Get Ready to Rumble’ I laugh as they do their dated dance moves and come over all nostalgic for PJ and Duncan. Then I felt a rumble of another kind, some pain which grew more intense, like how I imagine a concertina must feel when being squeezed in half, bloody hell this is it I realised and so I made ‘the call’ to husband, who drove back from wherever he was in jig time. “Get the bloody tens out” I screamed, having been a victim of chronic back pain my whole thirty years even I knew I needed back up. Now I’m all business, managing the tens machine with one hand and my contraction app with the other, both a great distraction from the reality that I was going to have a baby and soon! With all my tech I felt I could rule the world, I was in control, I knew what was going on. Clearly these women who surprise deliver on the toilet never had HG, how could you not know you were pregnant in the first place?
I was so agitated I couldn’t think straight. I was only comfortable laying bent over a chair, I must’ve looked so graceful. I know it’s time to ring the labour ward but midwife tells me I don’t sound like I’m in labour (I’ve always had a good telephone voice) so I soldier on. A trip to the loo and I have ‘a show’ – time to go! Suddenly realise the Husband only has a coupe and I literally can’t sit on my arse so I clamber into the back seat and kneel with my arms hugging the head rest, face squashed up against the tiny rear window. Some poor sod at the red lights think’s I’ve been trafficked. We made it to the hospital which was in the midst of a massive refurbishment so we have to walk round the back of the building to the labour ward, I recall this was not fun as I stop for a contraction to pass and to puke.
I think I’m going to shit myself and go to the toilet as soon as we get there, and it’s carnage with blood everywhere. I think I’m going to die, then I remember this is supposed to happen. Midwife states she’ll need to examine me to see how many centimeters dilated I am and asks me to lay down. I’m adamant I cannot lay down, and ask ‘if we can do it standing up’. She doesn’t know how to take this request and I spy husband trying not to laugh.
I’m five fucking centimeters! I’m off to deliver. Birth plan goes out the window, no water birth for me so I remain as I have done for hours, on my knees. I hear husband at the business end ask the midwife ‘what’s that?’ – ‘Piles’ she casually replies. Classy to the end. Three hours of pushing and the threat of a c section under general anaesthetic which I point blank refuse results in a forceps delivery but finally he is here. Hubble has entered our world. We didn’t actually name him Hubble but the thought did cross my mind. He lay on my chest and we marvel at our miracle. I have some tea and digestive biscuits and I don’t feel sick one little bit, I have third degree tears but no sickness or nausea. You can’t have it all.
The thing with hyperemesis is physical illness aside - the mental torture is just, if not equally as bad. Have a baby they said, you'll glow they said.
The only glow from me was a shade of puke green. To this day, I can vomit just brushing my teeth, my gag reflex is super sensitive (ask my dentist and my husband) again poor guy! When Kate - Duchess of Cambridge was pregnant and hyperemesis made the media I physically threw up. I felt the nausea like it was happening to me. Smells, songs, places can trigger it. It's like puke PTSD and still people ask, 'have you tried ginger'? Jesus Christ how I'd have punched these people if only I had the energy to make a fist. I tried the lot, all the cheap meds, travel sickness bands, two on each wrist, it was a fetching look, very Wimbledon, dry crackers, ginger bastarding biscuits but nothing worked. Mint humbugs helped for a bit - reduced the saliva output for a while then I was sick of them too.
I wanted the glow, to be on mat leave doing pre-natal Pilates and lunching around town picking out things for the nursery, but no! I lay in bed graduating to the sofa on a good day, permanently in pjs, make up less and mojo less (saved a fortune on cosmetics - so much so I bought the husband a Rolex). Sick pay had a whole new meaning. He did alright out of it really.
Ask anyone who's had HG and they'll tell you the same, they felt robbed. Robbed of the pregnancy they'd dreamt of, longed for and that's a hard pill to swallow.
Today I am not the woman I once was, yet now four years down the line I find myself hankering for another, a sibling for my HG hero who I love with all my heart, who was worth every puke, every pill, every pile and who despite it all is pure perfection. We endured it together, we were a team from the start, we have a special bond, we made it. I'm still stunned that somehow during my HG hell I managed to keep him safe inside. Not only does he know the sound of my heart from the inside, he knows a good puke when he hears one.
So what now? Do I gamble, do I risk it all, my health, my sanity?
Have a baby they say,
You'll glow they say
Maybe…
I say.
'Fifty Shades of Green' Written by Christine Howie -
HG Survivor and Pregnancy Sickness Support Volunteer
HG Heroes - Dr Tony Nicoll
Dr Tony Nicoll of Dundee, Scotland, is my medical HG hero! He is an extraordinary person and I am delighted that he recently won a gold award in the ‘Outstanding Individual (Non-Clinical)’ category of the NHS Tayside Staff Appreciation and Recognition (STAR) Awards. I struggle to imagine that there could possibly be a more deserving winner.

Dr Nicoll always goes above and beyond to ensure that every patient under his care is thoroughly looked after. He is an expert in the treatment of HG (hyperemesis gravidarum) – amongst many other things! - and in applying his knowledge he is consistently calm, warm, sympathetic, trustworthy and reassuring. He truly wants to help hyperemesis sufferers suffer less, and is genuinely concerned for his patients’ physical and emotional well-being.
Without Dr Nicoll’s unfaltering care I am not sure how I would have survived my second pregnancy!
My First Pregnancy
In 2009 I was pregnant with my first baby and suffering severely with HG. In spite of being completely bed bound with no quality of life and unable to even turn my head or talk without being sick for months on end I was repeatedly told by several medical professionals that my sickness was ‘normal’. Not one of them checked my urine for ketones or suggested rehydration via IV fluids during the first few months, and the battle at any point for effective medication was pointless and distressing.
Over and over again I was made to feel guilty for considering any medication during pregnancy – of course I didn’t WANT to have to take medication, but having your body in starvation mode and being unable to do anything but lie still in a dark room battling non-stop intense nausea/vomiting during pregnancy is also not healthy - for you or your baby!
Those dark months were utter hell, both physically and mentally. I knew no better so had to accept what I was told and battle on through the torture of 24/7 relentless sickness month after month. All day every day I would just countdown to when I was asleep as it was the only time I could escape the sickness. The fact that this is SUPPOSED to be one of a woman’s happiest times of her life makes HG all the harder to deal with, and when most people dismiss your symptoms as ‘morning sickness’, suggesting traditional (and useless!) remedies such as ginger, and crackers, etc. this makes things impossibly worse. It is NOT ‘acute morning sickness’! I was SO thirsty, and SO hungry - ALL THE TIME - and yet couldn’t drink or eat a thing, not even water, without throwing up. Even though I wasn’t keeping anything down I would still dry wretch or throw up bile. With no relief at any point. It was horrific.
Duchess of Cambridge
Three years later, when the Duchess of Cambridge fell pregnant for the first time, there were a few intense days when I did many interviews about HG for newspapers and radio stations and, crucially, the volunteer work I do with Pregnancy Sickness Support was also featured on STV news. It was watching this news article on the TV that helped me realise who I needed to speak to for decent care if I was to face being pregnant again to give Joseph, my first born, a sibling. My now hero, Dr Tony Nicoll, was featured in the same article giving the medical expert information and was clearly very ‘HG friendly’! I am not sure my little three year old Theo would be here today if it wasn’t for discovering this amazing doctor.
My Second Pregnancy
Seven months after this, I was pregnant for the second time, and the experience could not have been any more different to the first.
Undoubtedly I was much more knowledgeable myself which helped, but crucially I had the life-saving volunteers at Pregnancy Sickness Support and the remarkable care of Dr Nicoll on my side this time! I should say AT my side, as they – and he - were there every step of the way.
It was still a horrendous pregnancy but I got the best possible medical care and thanks to Dr Nicoll and P.S.S. (Pregnancy Sickness Support) I felt significantly less isolated, scared and miserable, and much more believed and understood.
Most vitally, Dr Nicoll treated my hyperemesis properly with IV fluids and medication from the beginning and therefore minimised the length and intensity of sickness as much as was possible. He is intelligent and experienced, and was always able to clearly explain everything to me at every stage.
From my pre-pregnancy planning appointments with Dr Nicoll, I could tell he took hyperemesis seriously and didn’t just shrug it off as ‘morning sickness’. I had taken along a great HG medical protocol written by the brilliant Dr Marjory McLean (another Scottish HG medical hero!) to my pre-pregnancy appointment as I was prepared that the mention of medication just might be shrugged off again - but this was absolutely not the case. Dr Nicoll knows how to treat HG and it is not with crackers or ginger biscuits!!!
I was terrified and devastated at the thought of being pregnant and having HG again, especially as it would mean I wouldn’t be able to be a proper mum to my son Joseph for so many months, but Dr Nicoll alleviated a lot of my fears.
Once the hyperemesis struck he had it arranged that I could go into Ninewells hospital as a day patient for two bags of IV fluid whenever required - and directly, without going through a GP, and there was never a battle for the medication I needed.
We had a sensible step by step plan set out before pregnancy - and in writing - so I wasn’t left in doubt as to whether I would get the care Dr Nicoll had approved if he happened not to be at the hospital when I needed treatment.
During my pregnancy he also arranged for extra reassurance scans which were obviously comforting but also provided some much needed, encouraging, positive moments in amidst the torturous sickness!
He made the hell of HG so much more bearable in so many ways. To know that you will be taken seriously and treated properly makes such a difference, especially at a time when you are extremely weak and vulnerable. I know, as a P.S.S. volunteer who has supported others under Dr Nicoll's care, that he has been exceptional with all of them too. The difference in these ladies, both physically and emotionally, once they are under Tony’s care, is indescribable.

Star Awards
In nominating Dr Nicoll for a STAR award I came to learn that not only is he exceptional at treating hyperemesis gravidarum, he is just simply truly exceptional - in all his fields of work.
Everyone I have spoken to about him seems to have heard of him and also speak about him in a super hero sort of way!
Unfortunately great care for hyperemesis is rare, but Dr Nicoll sets the perfect example to others of how to treat those suffering with the condition – with seriousness, compassion, understanding and care. I really hope Dr Nicoll realises what an impact he has had on my, and my family’s life. He is so gracious and modest that I’m not sure he will! Even more so, I hope that other doctors follow his outstanding example.
My Other HG Heroes...
This post was primarily to highlight Dr Nicoll’s amazing work, but, with deep emotion, I must also mention a few more heroes…
My family (I am so grateful for you) and also friends (all of you who helped and most especially the extreme kindness and compassion from Monika, Ruth and Alexis) who did so much.
Then there is Caitlin Dean, who runs Pregnancy Sickness Support… an absolute SUPERHERO! Without Caitlin I am almost certain that I would never have been able to face going through a second pregnancy, and my little Theo would not be here. I wish I had your intelligence and eloquence to put into words how grateful I and the world of hyperemesis sufferers are for your tireless efforts. You are truly unique.
Also, another amaaaaaazing hero - Lyle Brooks in New York, who runs Beyond Morning Sickness. Once again, I am lost for words as how to describe your caring, hardworking and generous nature, and how grateful the hyperemesis world is for you.
The amazing Kimber Wakefield MacGibbon who founded the HER Foundation in America as without her website (http://www.hyperemesis.org/) I don’t know how I would have gotten through my first pregnancy
Lastly, I am sending a huge thank you to all of the Pregnancy Sickness Support volunteers and also previous sufferers from right around the world who supported me through that second pregnancy. There were so many of you bombarding me with messages of support and I will never forget you doing that! It meant, and means, so much. Thank you, all of you HG heroes, from me and my little HG survivors, Joseph and Theo.

"Being able to provide pregnancy care for women and their families is something that I am very proud of and I feel very lucky to be able to be a part of so many life changing moments.
I aim to continue to provide high quality care to women in Tayside and I will do my best to ensure that every pregnant woman that I look after has the best experience possible." - Dr Tony Nicoll
-Dr Tony Nicoll was nominated as an HG Hero by Heather Miranda
- To raise money for Pregnancy Sickness Support Heather's son Joseph will be busking on his violin and electric piano in Dundee over the summer. You can support Joseph by following this link and donating what you can http://uk.virginmoneygiving.com/Joseph_PSS
THE JOY OF HG
Happy Father's Day!
In celebration of Fathers Day yesterday i asked Ian to write a guest blog to raise awareness of what it is like for husbands and partners supporting their wives/partners through HG.... Here's to the Joy of HG

Finding out your partner is pregnant is one of the most incredible things that can happen to you.
I found myself overjoyed and excited at the prospect of my then fiancé and soon to be wife growing our child within her. The expected ongoing joy and excitement of 9 months of waiting for the new baby boy or girl to arrive. My partner glowing with pregnancy and happy to be carrying our child, although evidently concerned with the arrival process!
Sadly none of this was to be the case beyond a couple of weeks.
Around week 4 we were pregnant by week 6 she was vomiting endlessly. Unable to hold down toast or even water. I witnessed her glow diminish and her shrink in size. Spending my time concerned for her wellbeing instead of excited for our child’s arrival. I effectively nursed her when I was home, and during the week when I was at work I worried incessantly as to whether she was ok, had she managed to eat or drink. Had she managed to go an hour without vomiting?
Being called to be told she is in hospital and on a drip to try and re-hydrate her is not a nice call to take. This call multiple times is horrendous.
She probably should have been in hospital more but stubbornly refused to go.
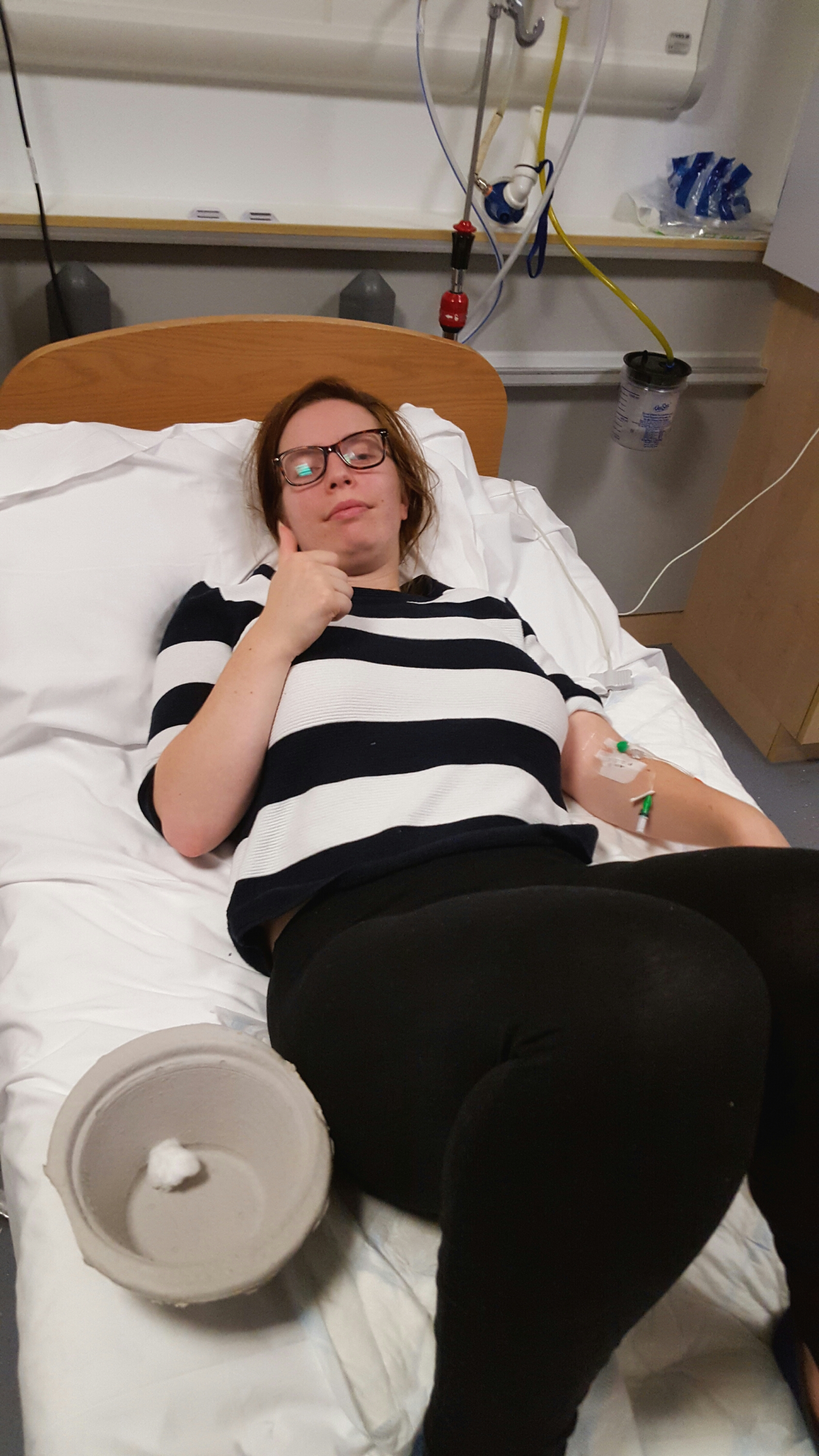
Most women seem to enlarge when pregnant. This is natural; there is an additional person in there! Not my wife, she continued to fade away. She was able to do less and less and I worried more and more for her and the baby. Maintaining a positive and strong stance in front of her whilst internally being frightened is not fun!

Having no one to engage with about the problem, as no one else could possibly understand the situation meant I had to deal with all of the challenges and worries on my own internally.
There was no free time. I either worried and looked after her, or worried and strived to get home to look after her.
The pregnancy could not pass quick enough. The sooner the baby arrived the sooner my wife could recover. Why was she so ill? No one seemed to have an answer other than ginger biscuits or some other ridiculous old wives tale.
Fortunately she did survive, we had a beautiful daughter and I could finally relax, as she regained strength and became herself again.
The zombie was once again being replaced by my vibrant and feisty wife.
So we decided to have another child. It couldn’t be as bad surely! Of course it could, and it was. Fortunately this time the Dr’s understood the condition and she was prescribed some heavy hitting ant-sickness drugs. This did not prevent her from once again withering down and ending up in hospital.
When not in hospital struggling to cope with our eldest daughter, as activity was too much and she was unable to cook as it made her violently ill.
I once again had to deal with the emotional challenge of supporting a very ill wife whilst at home and away for prolonged periods. Dealing with a situation by phone, when all I wanted to do was be at home.
Again I had no one to talk too as still no one else could understand my situation and my emotional struggle.

My wife was not to see the struggle I went through as I did not want her to worry, when the priority was keeping her as well as possible and positive.
Fortunately the second time she had support from mental health midwives and PSS which greatly helped her, and for that I am grateful.

Perhaps husbands need to acknowledge they need support as well, not all the time but every now and then just some re-assurance so you can maintain the positive persona for your sick partner.
I did not share my feelings with my partner so as not to upset her, and get her down. This perhaps was a mistake. My wife being an emotional creature felt more alone without my feelings and fears, and as if she was not understood. I as a very much task, not emotional person find it hard to engage emotionally and see the positive show as primary. What is best is communication, understanding and support.
Hopefully in the future more men will realise this and reach out to potential support groups and not see it as a failing or weakness. It takes strength to engage, and open up with your problems. Women understand that some men may not be emotional creatures and therefore what you perceive as simple sharing of feelings will ease a problem is something which is beyond your task orientated partner.
Communicate and support for each other is key! Pregnancy I’m afraid for the HG suffering couple is not pleasant. It is something to deal with and defeat prior to the joy of a new born child and the recovery of the partner you love.

For further information and support please contact Pregnancy Sickness Support by Phone: 02476382020 or Email: [email protected]
A Narrative Research Project
For those of you new to my blog I'm currently undertaking a PhD in Health Studies focusing on hyperemesis gravidarum to help further the international research efforts. PhD's are fairly long and arduous processes and a hell of a lot slower than my usual pace of churning out surveys of women's experiences and so on. But, the research produced is of a far higher quality and therefore has a much greater impact on the world of evidence based medicine.
As part of my PhD I'm conducting a Narrative research project and after a long process of developing the protocol, applying for ethical approval and piloting it... then having to apply for an adjustment of ethics. Anyway, its now ready! so if you are interested in taking part please re on.....
The Impact of Hyperemesis Gravidarum on Women's Reproductive Lives - A Narrative Research Project
Have you experienced a pregnancy affected by Hyperemesis Gravidarum (HG)? Do you want to tell your story for research?
 HG researcher, Caitlin Dean, in conjunction with Plymouth University, is recruiting women to take part in a project to explore women’s experience of HG and how it has impacted their reproductive lives. If you have had one or more pregnancies affected by HG you may be eligible to take part.
HG researcher, Caitlin Dean, in conjunction with Plymouth University, is recruiting women to take part in a project to explore women’s experience of HG and how it has impacted their reproductive lives. If you have had one or more pregnancies affected by HG you may be eligible to take part.
We are looking for women willing to share their whole HG story, from beginning to end including any potential affects in the future. You can either write or type your story in your own time or you can tell the researcher, Caitlin, your story over the phone, via skype or face-to-face (depending on location). If you choose to tell your story by phone, skype or face-to-face it would be recorded and transcribed. After this Caitlin may get in touch with you again to clarify parts of your story or ask you to expand on aspects. For full details of what is involved please click here.
To be able to take part you need to live in the UK and be over 18 years old.
We want to ensure that women from all sorts of backgrounds are represented and that the women interviewed represent the diversity of pregnant women in Britain today. To ensure this we are asking women interested in taking part to fill in an online form giving us some details about themselves.
Hopefully everyone who wants to take part will be able to but if a lot of women apply then we may not be able to include everyone in the research. We will contact you within one week to let you know if you are able to take part.
Please click here to apply to participate in this research.
Blog archive
2017August 2017 (1)July 2017 (1)June 2017 (2)May 2017 (1)February 2017 (1)January 2017 (5)2016November 2016 (1)October 2016 (1)September 2016 (4)August 2016 (1)July 2016 (1)June 2016 (3)April 2016 (2)February 2016 (2)January 2016 (1)2015December 2015 (2)November 2015 (1)October 2015 (1)September 2015 (1)August 2015 (1)July 2015 (3)June 2015 (5)May 2015 (3)April 2015 (3)March 2015 (3)February 2015 (5)January 2015 (3)2014December 2014 (1)November 2014 (4)October 2014 (4)September 2014 (3)August 2014 (4)July 2014 (3)June 2014 (2)May 2014 (5)April 2014 (5)March 2014 (5)February 2014 (4)January 2014 (5)2013December 2013 (6)November 2013 (6)October 2013 (10)September 2013 (5)July 2013 (1)June 2013 (1)April 2013 (1)March 2013 (2)February 2013 (1)2012December 2012 (1)June 2012 (1)February 2012 (1)2011December 2011 (1)November 2011 (1)October 2011 (1)September 2011 (1)July 2011 (2)June 2011 (1)May 2011 (6)April 2011 (1)The Book

The Kids Book

About Me
 I am mother of three beautiful children and wife to a fantastic and supportive husband. I am a nurse, a farmer and a trustee for Pregnancy Sickness Support. I love working hard and spending time with my kids.
I am mother of three beautiful children and wife to a fantastic and supportive husband. I am a nurse, a farmer and a trustee for Pregnancy Sickness Support. I love working hard and spending time with my kids.
About this blog
Information and support for pregnancy sickness and hyperemesis gravidarum. Views are my own and do not represent those of any other organisation. Information provided here should not be a substitute for medical advice. My aim is to raise awareness and encourage sufferers to know they are not alone.
Previous award nominations



Archive
Explore past posts:
2017August 2017 (1)July 2017 (1)June 2017 (2)May 2017 (1)February 2017 (1)January 2017 (5)2016November 2016 (1)October 2016 (1)September 2016 (4)August 2016 (1)July 2016 (1)June 2016 (3)April 2016 (2)February 2016 (2)January 2016 (1)2015December 2015 (2)November 2015 (1)October 2015 (1)September 2015 (1)August 2015 (1)July 2015 (3)June 2015 (5)May 2015 (3)April 2015 (3)March 2015 (3)February 2015 (5)January 2015 (3)2014December 2014 (1)November 2014 (4)October 2014 (4)September 2014 (3)August 2014 (4)July 2014 (3)June 2014 (2)May 2014 (5)April 2014 (5)March 2014 (5)February 2014 (4)January 2014 (5)2013December 2013 (6)November 2013 (6)October 2013 (10)September 2013 (5)July 2013 (1)June 2013 (1)April 2013 (1)March 2013 (2)February 2013 (1)2012December 2012 (1)June 2012 (1)February 2012 (1)2011December 2011 (1)November 2011 (1)October 2011 (1)September 2011 (1)July 2011 (2)June 2011 (1)May 2011 (6)April 2011 (1)Online recommendations
- Best Non Gamstop Casinos 2025
- UK Casinos Not On Gamstop
- Casinos Not On Gamstop
- UK Casinos Not On Gamstop
- Non Gamstop Casino
- Best Betting Apps
- Best Non Gamstop Casinos
- Gambling Sites Not On Gamstop
- Non Gamstop Casino Sites UK
- Slot Sites Not On Gamstop
- Casino Not On Gamstop
- Best Non Gamstop Casinos
- Best Casino Sites Not On Gamstop 2025
- Non Gamstop Casinos
- Casino Sites UK Not On Gamstop
- Non Gamstop Casino UK
- Non Gamstop Casino UK
- Non Gamstop Casinos
- Slots Not On Gamstop
- Slots Not On Gamstop
- UK Casino Sites Not On Gamstop
- UK Casinos Not On Gamstop

